Understanding Base of Thumb Arthritis
What is base of thumb arthritis?
Base of thumb arthritis, also known as osteoarthritis of the 1st carpo-metacarpal joint (where the metacarpal bone of the thumb meets the trapezium bone in the wrist), is a common condition that typically develops as we age. It occurs when the smooth cartilage covering the ends of the bones in this joint breaks down, causing the bones to rub together. While osteoarthritis can develop at any age, it is most commonly seen in people over the age of 45, and it may run in families. A previous fracture in this joint can also contribute to the condition. Women are more likely to develop arthritis at the base of the thumb compared to men.
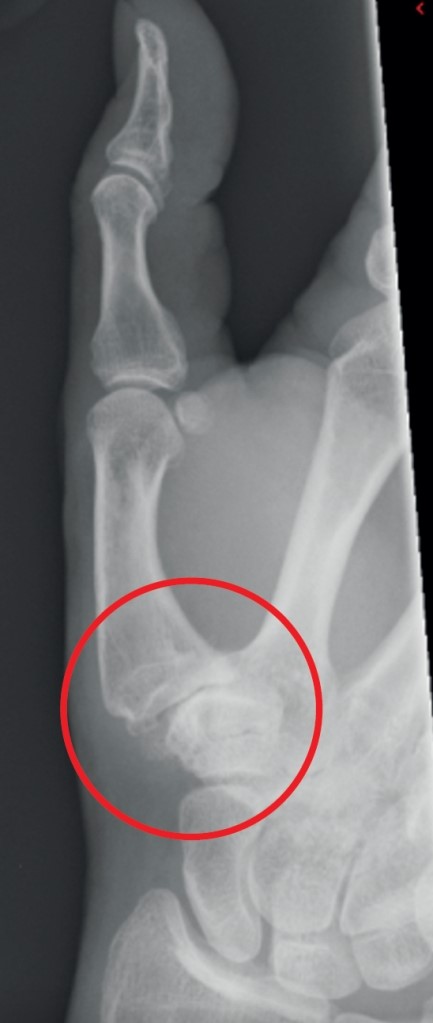
X-rays often show that around 60% of women over 60 have this type of arthritis, though not all experience significant pain. Typical signs of osteoarthritis on an X-ray include joint space narrowing.
What are the symptoms?
Pain at the base of the thumb, especially when using the thumb.
Tenderness when pressing on the base of the thumb.
Difficulty performing tasks that require thumb movement, such as opening jars or turning a key.
Stiffness in the thumb, with some loss of mobility, especially in terms of separating the thumb from the hand.
In more advanced cases, a bump may develop at the base of the thumb, and the middle joint of the thumb may hyperextend, causing a zigzag appearance.
What is the natural history?
The natural course of base of thumb arthritis is that pain often decreases or “burns out” over time, even though the arthritis itself remains. This means that while the condition doesn’t improve or heal, the associated symptoms, like pain, may subside over several years. Older individuals may have this condition but rarely complain of ongoing pain. In fact, using the thumb normally, even when it hurts, does not cause harm to the joint. The condition is typically self-limiting, and pain usually becomes more manageable over time.
It’s important to note that pain in arthritis serves as the body’s natural warning system. Though osteoarthritis pain can cause concern, in most cases, the condition does not worsen significantly over the years.
How can it be treated?
Treatment for base of thumb arthritis focuses on managing pain, as the arthritis itself does not require direct treatment. It’s important to remember that all treatments carry some level of risk, but major issues are rare. The following options are available for pain relief:
- Activity Modification – Adjusting how you perform certain tasks can help alleviate pain. There’s no need to avoid activities entirely, as using the hand in the presence of pain won’t worsen the arthritis.
- Splints – A rigid splint can provide support but may make thumb movements more difficult. A flexible neoprene splint can be a more practical option for daily use. Some rigid splints allow normal wrist movement while offering thumb support.
- Physiotherapy – Regular physiotherapy exercises can help maintain movement and reduce stiffness.
- Simple Painkillers – While painkillers can offer temporary relief, they are not a long-term solution. Log-term use of painkillers like ibuprofen can lead to side effects such as stomach ulcers or heart and kidney issues, and stronger painkillers may be addictive.
- Steroid Injections – A steroid injection can provide short-term pain relief by reducing inflammation in the joint. However, the relief is usually temporary, and the injections come with potential risks.
- Surgery – Surgery is typically a last resort, as non-surgical treatments often help manage symptoms over the long term. However, if symptoms are severe or persistent, surgical options may be considered. The most common surgical procedures include:
– Trapeziectomy: Removal of the trapezium bone, which has a good success rate for pain relief. However, this procedure weakens the thumb and reduces stability, so it’s important to weigh the benefits of pain relief against the potential loss of thumb function.
– Joint Fusion: Fusing the joint can provide good pain relief, particularly for younger patients with more manual jobs. However, this procedure restricts thumb mobility significantly, and the results can vary, with a relatively higher risk of complications.
In making a decision about surgery, it’s important to carefully consider the all the potential risks and benefits in discussion with your surgeon.

















